Flatfoot
Understanding Flatfoot
Flatfoot is a condition where the arch on the inside border of the foot is flat rather than raised causing the foot and toe to turn out and the ankle to roll inward. Although there are several types of flatfoot, such as rigid and flexible flatfoot, they both have a common factor: partial or complete loss of the arch. The posterior tibial tendon serves as one of the major supporting structures of the arch. This tendon descends the leg, runs along the inside of the ankle, and down the side of the foot. When it overstretches or becomes inflamed, it often results in the flattening of the foot known as posterior tibial tendon dysfunction (PTTD). Health factors such as obesity, diabetes, and rheumatoid arthritis may increase the risk of developing flatfoot.
The term “flexible” means that the foot is flat when standing and returns to a normal arch in non- weight bearing positions.
The term “rigid” means that the arch stays flat or collapses even without weight pressure.
Symptoms
Common symptoms of flatfoot are:
• Ankle turned inward
• Weakness/fatigue felt in the foot or leg
• Pain felt in the shin
• Pain in the heel, arch, ankle, or along the outside of the foot
Treatments
Before considering surgery, there are always non-operative treatments such as:
• Shoe modifications
• Orthotic devices
• Medications
• Immobilization
• Physical therapy
Custom orthotics, arch supports prescribed by a foot and ankle specialist, are made individually for each patient and can be helpful in reliving symptoms. Each custom orthotic is specifically made from an impression of the patient’s foot. Long-term arch support with a reduction in symptoms is the main goal of custom orthotics.
When non-operative solutions are no longer able to control the pain and disability, surgery becomes a reasonable option. Surgical options include:
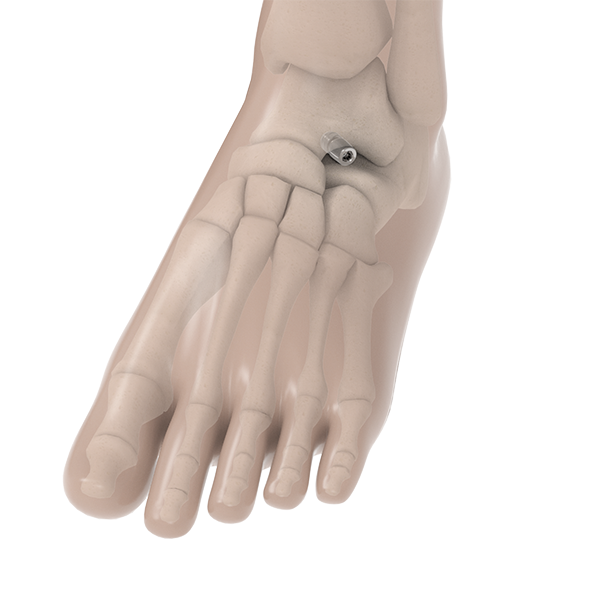
Arthroereisis – An implant is inserted within the sinus tarsi, which is the opening on the outside of the foot in between the ankle and heel bone. This restricts excessive joint rotation outward and creates an arch in the foot.
Arthrodesis (Fusion) – The cartilage surfaces of the joint are removed and a device such as a screw, plate, staple, etc. is utilized to prevent motion. The bones eventually fuse together which prevents pain; however, a loss of function occurs as the joint no longer functions. With this loss of function, your gait, or way of walking may change, which may affect other joints such as knees, hips, spine, etc.
Osteotomy – The bones are cut and reshaped to correct alignment.
Why the Subtalar Implant?
The BioPro® Horizon Subtalar implant acts as an internal orthotic, similar to wearing an orthotic within your shoe. The implant blocks excessive joint motion, maintaining the arch in your foot. The BioPro implant is designed with a smooth surface for your bones to rest against. This helps prevent any inflammation or bone erosion that is sometimes associated with this type of procedure.
The surgical procedure for the BioPro® Horizon Subtalar Implant usually lasts about 15 minutes. Before leaving, your surgeon is urged to also take an overhead X-ray to ensure that the placement of the internal orthotic is correct.
Most patients have a quick recovery and are walking the same day of surgery or the following day. Patients may also require the use of a walking boot to help provide support to the operated area.
Other information:
Please note: the benefits of short surgery time and recovery are related to the arthroeresis procedure using the BiopPro® Horizon Subtalar Implant only. Oftentimes, this is done in conjunction with other procedures. If you are having more than one surgery, you must follow your surgeon’s prescribed post-operative protocol after surgery.
What to expect after flatfoot surgery
After surgery the surgical site should remain numb for approximately six to eight hours. It is important during your recovery to elevate your foot. The application of ice to the surgical site is another effective post-op tool that will aid in minimizing inflammation and pain. Within 10 days of your surgery you should return to your physician for a post-op visit. Between 4 to 6 weeks patients usually return to the majority of their daily activities. After 2 to 3 months, minimal soreness may still be present in some patients and may be reduced by applying ice.
Learn what treatments may be right for you.
Find a Surgeon
Fill out the contact form or call us at 810-982-7777 to see if there is an experienced surgeon in your area.
Consult with your surgeon
Discuss all your possible treatment options and expectations after surgery.